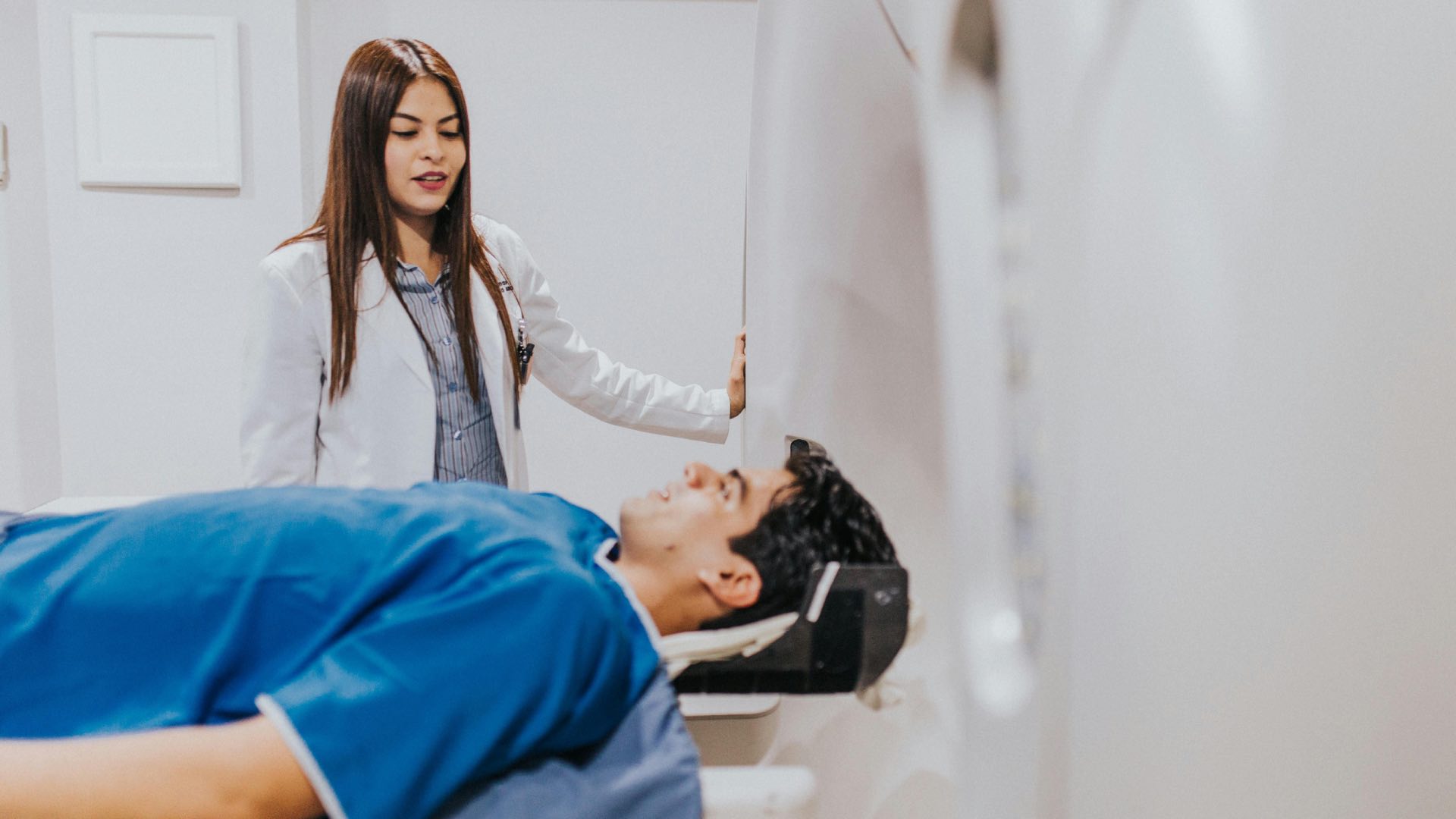
He was already said to be doomed by two serious illnesses. Yet, this 63-year-old man is now in complete remission from both HIV and cancer - an outcome made possible by a series of coincidences so extraordinary that even his doctors are still struggling to grasp their significance.
HIV positive since 2006, diagnosed with cancer in 2017
The "Oslo patient," whose identity is being withheld, has been living with HIV since 2006. His viral load had been well controlled with antiretroviral therapy until then. However, in 2017, he received a new diagnosis: myelodysplastic syndrome, a particularly aggressive blood cancer that disrupts blood cell production in the bone marrow. Without a transplant, his life was virtually at risk.
The search for a donor with extremely rare characteristics
The medical team at Oslo University Hospital then began an intensive search for a compatible donor. Their initial strategy focused on identifying a donor carrying the CCR5-delta32 mutation, a rare genetic anomaly that confers natural resistance to HIV—a trait possessed by only about 1% of the Northern European population. Faced with the failure of this first approach, the doctors turned to the patient's older brother, hoping for a better genetic match.
A stunning discovery on the very day of the transplant
On the day of the transplant in 2020, doctors were stunned to discover that the donor brother himself carried the CCR5 mutation. A minuscule chance, in a region of the world where it affects only one in a hundred people. The patient himself summed up the situation with a striking phrase: "It was like winning the lottery twice."
A confirmed remission, two years after the operation
Post-operative analyses gradually confirmed the transplant's effectiveness. Two years after the procedure, the "Oslo Patient" discontinued his antiretroviral treatments under strict medical supervision. Subsequent tests then detected no further viral traces in his blood, intestines, or spinal cord. His case was officially detailed in a study published on April 13, 2026, in the journal Nature Microbiology.
One more name on a very short list
The "Oslo patient" joins a very small international list—the so-called Berlin, London, Düsseldorf, New York, City of Hope, and Geneva patients—all considered cured or in sustained remission from HIV following a bone marrow transplant intended to treat cancer. They all share the same characteristic: a donor carrying the protective CCR5 mutation, with the notable exception of the Geneva patient, whose case explores other mechanisms.
A medical hope, but not a treatment that can be widely used
However, the researchers and physicians involved urge extreme caution. Bone marrow transplantation remains a complex and risky procedure, associated with significant mortality and very serious side effects. Its mortality rate can reach 20% in certain circumstances. Nevertheless, these cases remain invaluable "living laboratories" for research, offering avenues for understanding the mechanisms that could one day allow us to control or even permanently eradicate HIV.
In summary, this patient, nicknamed "Oslo Patient," defies medical statistics. His story illustrates how certain therapeutic advances arise from exceptional circumstances, where biology, medicine, and chance intersect in an almost unrepeatable way.